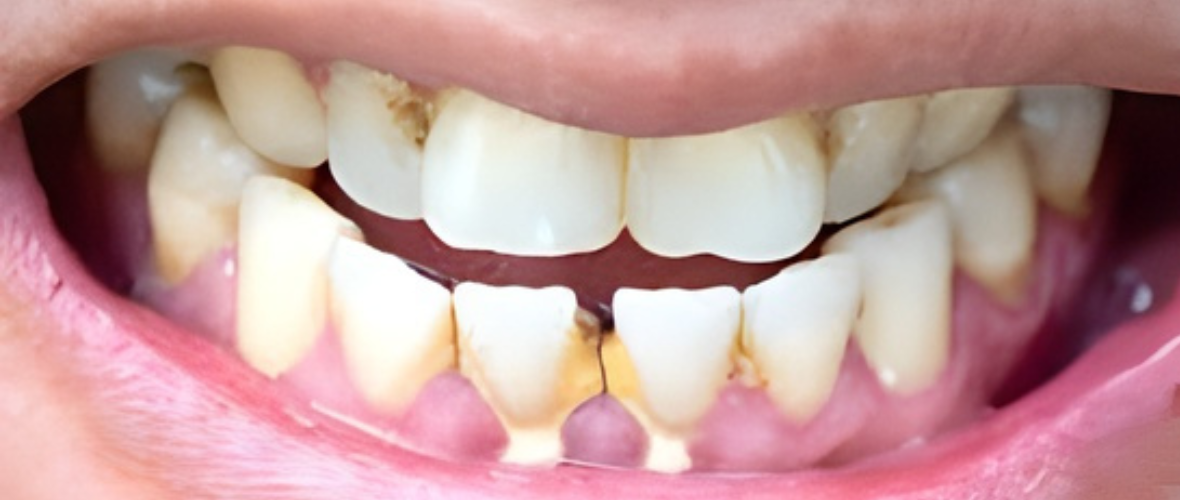
A calculus bridge represents one of the most concerning developments in oral health, yet many people remain unaware of its existence until it’s too late. This hardened deposit of dental plaque that spans across multiple teeth can have devastating effects on both your dental and gum health, potentially leading to serious complications if left untreated. Understanding what a calculus bridge is, how it forms, and its impact on your oral health is crucial for maintaining a healthy smile throughout your lifetime.
Understanding the Calculus Bridge: What Is It?
When hardened plaque accumulates and joins multiple teeth, a “bridge-like” structure known as a calculus bridge, tartar bridge, or dental calculus forms.. This condition involves the accumulation of dental calculus that spans over several teeth, forming a continuous band of hardened deposits that can be extremely difficult to remove.
Calculus is mineralized dental plaque. When soft plaque remains on your teeth without proper removal, it begins to harden through a process called calcification, which usually starts between the first and fourteenth days of plaque formation. The minerals in your saliva, primarily calcium phosphate, react with the bacterial plaque to create this rock-hard substance.
The formation process is quite rapid—calcifying plaques may become 50% mineralized in just 2 days and 60% to 90% mineralized within 12 days. This explains why consistent daily oral hygiene is so critical for preventing calculus formation.
The Formation Process: How Calculus Bridges Develop
Understanding how calculus bridges form helps explain why they’re so problematic for oral health. The process begins with dental plaque, a sticky film composed of bacteria, food particles, and saliva that naturally forms on teeth after eating. When plaque isn’t adequately removed through brushing and flossing, it begins to mineralize.
Key factors contributing to calculus bridge formation include:
Poor Oral Hygiene: Inadequate brushing and flossing are the primary culprits, allowing plaque to accumulate and harden.
Dietary Habits: Frequent consumption of sugary and starchy foods increases plaque formation, as bacteria feed on these substances to produce acids.
Smoking and tobacco use contribute to higher rates of tartar buildup and create conditions that promote calculus formation.
Individual Saliva Composition: Differences in saliva can affect how quickly plaque calcifies into tartar.
Dry Mouth Conditions: Reduced saliva flow means less natural cleaning action, allowing plaque to accumulate more rapidly.
Crystalline calcium phosphate salts are precipitated after calcium ions bond to carbohydrate-protein complexes in the organic matrix during the calcification process. Saliva serves as the primary source of mineralization for calculus that forms above the gum line (supragingival calculus). At the same time, gingival crevicular fluid provides minerals for calculus below the gum line (subgingival calculus).
Visual and Physical Characteristics
A calculus bridge has distinct characteristics that make it identifiable, though early stages may be subtle. The bridge appears as a whitish-yellowish plaque that forms along the gum line across multiple teeth. This tartar buildup typically has a rough, porous surface that provides an ideal environment for additional plaque accumulation.
Common visual signs include:
- Visible hardened deposits connecting several teeth
- Yellow, brown, or whitish coloration of the tartar
- Rough texture along the gumline
- Staining that doesn’t come off with regular brushing.
The rough surface of calculus creates more surface area for new plaque to adhere to, leading to a continuous cycle of buildup that becomes increasingly difficult to manage without professional intervention.
Impact on Gum Health: The Gateway to Serious Problems
The relationship between calculus bridges and gum health is particularly concerning. Calculus buildup irritates and inflames the gums, leading to a cascade of problems that can ultimately result in tooth loss if not addressed promptly.
Gingivitis: The First Stage
Gingivitis, the early stage of gum disease, is usually the first sign of a calculus bridge’s negative effects on gum health. The hard, rough surface of calculus harbors bacteria that produce toxins, which enter the gum tissues and cause inflammation.
Signs of gingivitis include:
- Red, swollen gums that may appear puffy or enlarged
- Bleeding during brushing or flossing is often the first noticeable symptom.
- Tender gums that may be sensitive to touch
- Bad breath (halitosis) that persists despite oral care efforts
Since gingivitis is the only stage of gum disease that may be reversed, early detection and treatment are essential. However, when calculus bridges are present, simple brushing and flossing cannot effectively remove the hardened deposits, allowing the condition to progress.
Progression to Periodontitis
If gingivitis caused by calculus bridges remains untreated, it can advance to periodontitis, a severe form of gum disease that can destroy the gums and underlying bone structure. This condition represents a critical threat to oral health, as it can result in permanent tooth loss.
Periodontitis symptoms include:
- Deep pockets forming between teeth and gums
- Gum recession, exposing tooth roots
- Loose or shifting teeth due to bone loss
- Persistent bad breath and a metallic taste
- Pus formation around the gumline
Research has established strong associations between periodontitis and systemic health conditions, including heart disease, diabetes, and respiratory problems. This connection underscores the importance of addressing calculus bridges before they contribute to more serious health complications.
Effects on Dental Health: Beyond Surface Problems
While gum health often receives primary attention when discussing calculus bridges, the impact on dental health is equally significant. The presence of calculus creates an environment that promotes various dental problems, from aesthetic concerns to structural damage.
Tooth Decay and Cavities
Calculus provides the ideal circumstances for bacteria to proliferate and generate acids that can damage tooth enamel. The rough, porous surface of calculus traps food particles and bacteria, creating localized areas of high acidity that can lead to cavity formation.
The process works as follows:
- Bacterial colonization: The rough calculus surface attracts and harbors acid-producing bacteria
- Acid production: These bacteria metabolize sugars and starches from food, producing acids
- Enamel erosion: The acids attack tooth enamel, creating weak spots that develop into cavities
- Progressive damage: Without intervention, cavities can penetrate deeper into the tooth structure
Tooth Sensitivity
As calculus buildup contributes to gum recession, it can expose tooth roots that were previously protected by gum tissue. These exposed roots lack the protective enamel coating found on tooth crowns, making them particularly sensitive to temperature changes, sweet foods, and acidic substances.
The sensitivity occurs because:
- Dentin exposure: Root surfaces contain dentin, which has microscopic tubules leading to the tooth’s nerve
- Increased nerve stimulation: Hot, cold, or acidic substances can travel through these tubules to stimulate the nerve
- Reduced natural protection: Without gum coverage, roots remain vulnerable to environmental irritants
Aesthetic Impact
Beyond health concerns, calculus bridges create significant aesthetic problems that can affect self-confidence and social interactions. The deposits are often obvious, particularly when they form on front teeth or along the gum line.
Aesthetic issues include:
- Discoloration: Calculus easily absorbs stains from coffee, tea, tobacco, and food, creating unsightly yellow, brown, or black deposits
- Altered smile appearance: The buildup can make teeth appear uneven or create an obvious line of discoloration
- Bad breath: Persistent halitosis associated with calculus can impact social interactions and self-esteem
The Halitosis Connection: Understanding Bad Breath
One of the most socially impactful effects of calculus bridges is persistent bad breath, or halitosis. This condition affects approximately 2.4% of the adult population and can have significant psychological and social consequences.
The Science Behind Calculus-Related Bad Breath
Calculus bridges contribute to halitosis through several mechanisms:
Bacterial proliferation: The rough surface of calculus provides ideal conditions for bacteria to multiply and thrive. These bacteria, particularly anaerobic species, break down proteins and produce volatile sulfur compounds (VSCs) that create the characteristic unpleasant odor.
Tissue inflammation: The gum inflammation caused by calculus creates additional sources of bacterial growth and protein breakdown, contributing to odor production.
Food trapping: Calculus bridges create irregular surfaces and pockets where food particles can become trapped, leading to bacterial fermentation and odor production.
The primary volatile compounds responsible for halitosis include
- Hydrogen sulfide: Produces a rotten egg smell
- Methyl mercaptan: Creates a garlic-like odor
- Dimethyl sulfide: Contributes to the overall unpleasant breath
1. Impact on Quality of Life
Halitosis associated with calculus bridges can significantly impact personal and professional relationships. Studies show that people with persistent bad breath may experience:
- Social withdrawal and reduced confidence in interpersonal situations
- Professional limitations in careers requiring close personal interaction
- Psychological stress and anxiety about breath odor
- Relationship difficulties due to embarrassment or partner concerns
2 . Systemic Health Connections
Research has increasingly revealed connections between oral health problems like calculus bridges and overall systemic health. The bacteria and inflammation associated with calculus buildup don’t remain localized to the mouth but can have far-reaching health implications.
3 . Cardiovascular Health
Studies have shown associations between gum disease (often exacerbated by calculus buildup) and cardiovascular problems. The proposed mechanisms include:
- Bacterial translocation: Inflamed gums can allow oral germs to enter the bloodstream.
- Inflammatory response: Systemic inflammation may be exacerbated by persistent mouth irritation.
- Immune system activation: Persistent oral infections may trigger immune responses that affect cardiovascular health
4. Diabetes Management
The relationship between oral health and diabetes is bidirectional—diabetes can worsen gum disease, while gum disease can make blood sugar control more difficult. Calculus bridges contribute to this cycle by:
- Promoting persistent inflammation that can affect insulin sensitivity
- Creating bacterial reservoirs that maintain chronic infection
- Complications in oral hygiene efforts are necessary for diabetic oral health management.
5. Respiratory Health
Aspiration of oral bacteria, particularly in elderly individuals or those with compromised immune systems, can lead to respiratory infections. Calculus bridges increase this risk by:
- Harboring pathogenic bacteria in large quantities
- Creating persistent sources of bacterial contamination
- Contributing to the overall oral bacterial load
Treatment Options: Professional Intervention Required
Unlike regular plaque, calculus cannot be removed through home oral hygiene practices alone. The hardened nature of calculus requires professional dental intervention using specialized instruments and techniques.
1. Scaling: The Primary Treatment
Scaling represents the cornerstone of calculus bridge treatment. This procedure involves the mechanical removal of calculus deposits from tooth surfaces, both above and below the gum line.
The scaling process includes:
Manual scaling: Dental professionals use hand-held instruments called scalers to carefully scrape away calculus deposits.
Ultrasonic scaling: High-frequency vibrations break up calculus deposits, making removal more efficient and comfortable.
Subgingival scaling: For calculus below the gum line, specialized instruments access deeper areas to remove deposits from tooth roots.
2. Root Planing: Smoothing the Foundation
When calculus has formed below the gum line, root planing may be necessary. This procedure involves smoothing the tooth root surfaces to:
- Remove bacterial toxins that have penetrated the root surface
- Eliminate rough areas where bacteria can accumulate.
- Promote gum reattachment to cleaned tooth surfaces.
- Reduce pocket depths between teeth and gums.
3. Advanced Interventions
Other therapies can be required in extreme situations where calculus bridges have exacerbated gum disease:
Surgical intervention: Deep pocket reduction surgery or regenerative procedures may be required to restore gum health.
Laser therapy: Some dental practices use laser technology to assist in calculus removal and gum treatment.
Antimicrobial therapy: Antibiotic treatments may be prescribed to control bacterial infections associated with severe calculus buildup.
4. Prevention Strategies: Your Best Defense
Prevention remains the most effective approach to avoiding calculus bridges and their associated health problems. A comprehensive prevention plan addresses all factors that contribute to calculus formation.
5. Daily Oral Hygiene Excellence
Brushing technique and frequency: Brush teeth at least twice daily using fluoride toothpaste, with particular attention to the gum line where calculus commonly forms.
Effective brushing involves:
- Using a toothbrush with soft bristles can remove plaque efficiently and prevent gum damage
- Angling bristles toward the gum line to clean the area where calculus typically begins
- Using gentle, circular motions rather than aggressive scrubbing
- In order to guarantee complete cleaning, brush for a minimum of two minutes.
- Replace toothbrushes every three to four months.
Flossing daily: Regular flossing removes plaque from between teeth, where calculus bridges often begin. Proper flossing technique includes:
- Use about 18 inches of floss to ensure clean sections for each tooth
- Cleaning beneath the gum line involves wrapping floss around each tooth.
- Using gentle back-and-forth motions to avoid gum trauma
- Cleaning both sides of every tooth, including back molars
6. Antimicrobial Support
Mouthwash use: Antibacterial mouthwash can help reduce plaque-forming bacteria and provide additional protection against calculus formation.
Professional recommendations: Consult with dental professionals about prescription-strength antimicrobial rinses if you’re at high risk for calculus formation.
7. Lifestyle Modifications
Dietary considerations: Limiting sugary and starchy foods reduces the substrate available for bacteria to produce acids and contribute to plaque formation.
Hydration: Maintaining adequate saliva flow through proper hydration helps with natural mouth cleaning.
Smoking cessation: Eliminating tobacco use significantly reduces calculus formation risk and improves overall oral health.
Professional Care: The Essential Partnership
Regular dental visits play a crucial role in preventing calculus bridge formation and maintaining optimal oral health. Depending on each person’s unique risk factors, the frequency of professional treatment should be customized.
1. Standard Cleaning Schedule
For most people, calculus buildup can be avoided with an expert cleaning every six months. This schedule allows for:
- Early detection of calculus formation before bridge development
- Professional removal of calculus that may have formed despite good home care
- Assessment of oral health changes and risk factors
- Customized prevention recommendations based on individual needs
2. High-Risk Individuals
More frequent professional care, like as cleanings every three to four months, can be necessary for some people. High-risk factors include:
- History of gum disease or calculus formation
- Smoking or tobacco use
- Diabetes or other systemic conditions
- Dry mouth conditions from medications or medical treatments
- Orthodontic appliances that complicate home oral hygiene
3. Professional Assessment Benefits
Regular dental visits provide opportunities for:
Early intervention: Identifying and addressing calculus formation before it progresses to bridge formation.
Risk assessment: Evaluating individual factors that may predispose to calculus formation.
Technique improvement: Receiving personalized instruction on optimal home oral hygiene techniques.
Health monitoring: Detecting early signs of gum disease or other oral health problems.
The Cost of Inaction: Long-Term Consequences
Understanding the potential long-term consequences of untreated calculus bridges emphasizes the importance of prevention and early intervention. The progression from calculus bridges to serious oral health problems can be rapid and costly.
Financial Implications
Preventive care costs: Compared to treating more serious issues, routine cleanings and examinations need a much smaller financial outlay.
Treatment escalation: Thousands of dollars may be spent on advanced gum disease therapy, which may include surgery.
Tooth replacement: When calculus bridges contribute to tooth loss, replacement options like implants or bridges involve significant expense and time.
Quality of Life Impact
Functional limitations: Advanced gum disease can make eating difficult and limit food choices.
Aesthetic concerns: Social interactions and self-confidence may be impacted by visible calculus accumulation and its effects.
Health complications: The systemic health connections mean that untreated oral problems may contribute to other medical conditions.
Frequently Asked Questions
Q: 1. Is it possible for me to take out a calculus bridge on my own at home?
A: No, calculus bridges cannot be removed through home oral hygiene practices. The hardened nature of calculus requires professional dental instruments and expertise for safe and effective removal.
Q:2 How quickly can a calculus bridge form?
A: Calculus formation can begin within 2-3 days of plaque accumulation, with significant mineralization occurring within 12 days. Bridge formation depends on individual factors, but it can develop relatively quickly without proper oral hygiene.
Q: 3. Is a calculus bridge always visible?
A: Not always. While calculus above the gum line (supragingival) is often visible as yellowish-white deposits, calculus below the gum line (subgingival) may not be apparent without professional examination.
Q:4 Can calculus bridges come back after professional removal?
A: Yes, without proper ongoing oral hygiene and regular professional care, calculus can reform. This is why consistent daily oral care and regular dental visits are essential for long-term prevention.
Q: 5. Do I get gum disease if I have a calculus bridge?
A: Calculus bridges frequently cause gum disease and inflammation. If you have a calculus bridge, you probably have gingivitis, or early-stage gum disease, which needs to be treated by a dentist.
Q: 6 How often should I see a dentist if I’m prone to calculus formation?
A: Individuals prone to calculus formation may need professional cleanings every 3-4 months rather than the standard 6-month interval. Your dental professional can recommend the appropriate frequency based on your risk factors.
Taking Action for Your Oral Health
A calculus bridge represents more than just a cosmetic concern—it’s a serious threat to both dental and gum health that can have far-reaching consequences for your overall well-being. The hardened deposits create an environment that promotes gum disease, tooth decay, and bad breath, and potentially contributes to systemic health problems.
The good news is that calculus bridges are entirely preventable through consistent oral hygiene practices and regular professional dental care. By understanding the formation process, recognizing early warning signs, and taking proactive steps to maintain oral health, you can avoid the serious complications associated with calculus buildup.
Don’t forget that prevention is always cheaper and more efficient than treatment. Establishing excellent daily oral hygiene habits, making informed dietary choices, and maintaining regular dental visits creates the foundation for lifelong oral health. If you suspect you may have calculus buildup or haven’t had a professional cleaning in more than six months, don’t wait—schedule a dental appointment today.
Your smile, your health, and your confidence depend on the actions you take now to protect against calculus bridge formation. With proper knowledge and consistent care, you can maintain healthy teeth and gums throughout your lifetime, avoiding the serious consequences that calculus bridges can bring to your oral and overall health.